|
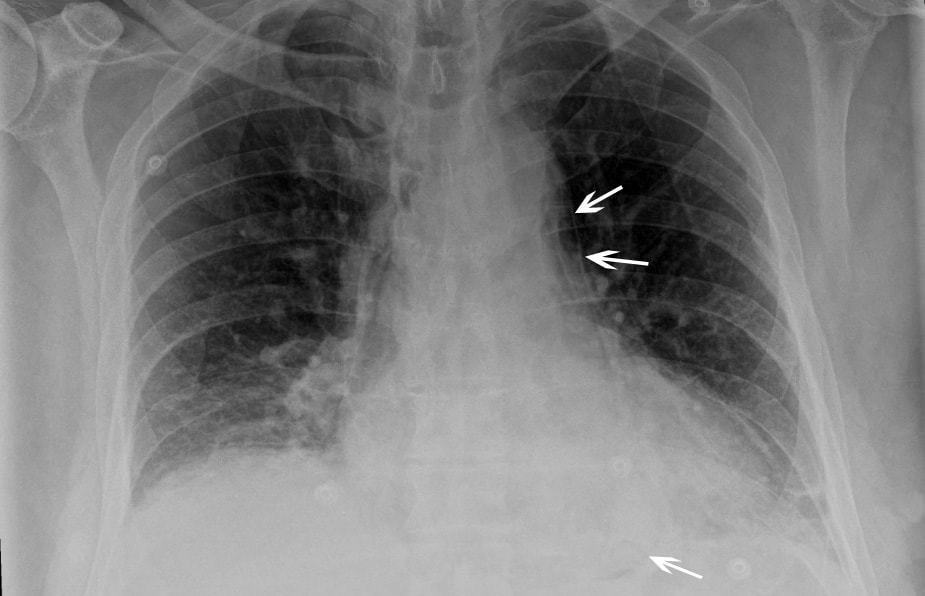
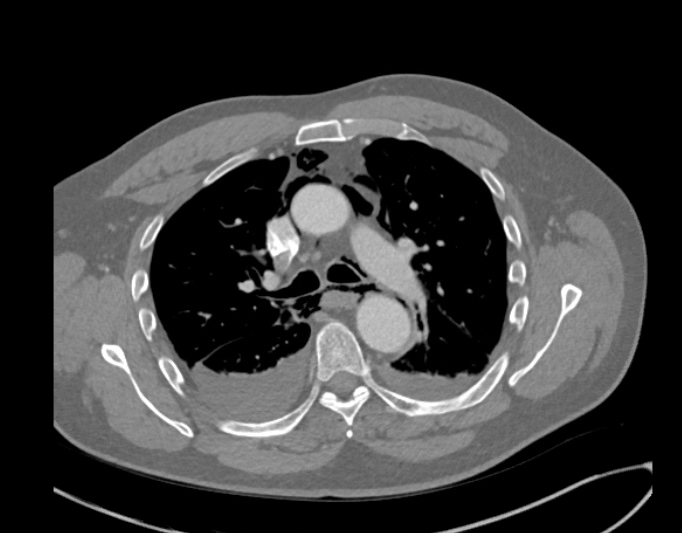
A patient presents to your department with worsening epigastric/chest pain after eating a chocolate bar. He felt a piece of the bar got stuck low down in his chest and he had been retching afterwards. His pain has been getting worse through the day and on arrival he is tachycardic, tachypneic and slightly hypoxic. He is able to swallow fluids, but despite large doses of IV morphine he remains uncomfortable. An arterial blood gas done by one of your colleagues shows mild type 2 respiratory failure and you are asked for advice. You go and review the patient and the investigations. Despite large doses of analgesia, the patient remains very uncomfortable and is reluctant to take deep breaths. On the CXR you note a subtle double line at the right side of the mediastinum and possible similar in the pericardium. See arrows on the CXR: You suspect a pneumomediastinum and order a CT chest/abdomen +/- contrast. This confirms widespread mediastinal air suggestive of lower oesophageal perforation confirming your clinical suspicion of Boerhaave Syndrome. His hypoxia and type 2 respiratory failure can be explained by underventilating due to the severe pain. CT image from the same patient, reported as: ‘Extensive pneumomediastinum, subcutaneous emphysema and bilateral pleural effusions with lower lobe consolidation. The appearance is suggestive of Boerhaave Syndrome.’ What is Boerhaave syndrome? Spontaneous rupture of the oesophagus, caused by forceful vomiting/retching. First described in 1724 by the Dutch physician Herman Boerhaave who diagnosed the condition in Jan van Wassenaer, a Grand Admiral of the Dutch Fleet who died 24hrs after vomiting, having feasted on a sumptuous meal with copious amounts of wine.* Pathophysiology: Spontaneous oesophageal rupture is caused by a sudden rise in internal oesophageal pressure produced during vomiting. The most common site of the perforation is in the lower third of the oesophagus. Symptoms: The classic triad of vomiting, chest pain and subcutaneous emphysema is only present in 14% of presentations. Other symptoms are upper abdominal pain, dyspnoea, tachypnea, odynophagia. The symptoms are often mistaken for other pathologies, e.g. myocardial infarction, chest infection. Diagnosis: is suspected on CXR by the presence of pneumomediastinum, and sometimes a pleural effusion and/or pneumothorax. A CT scan, ideally with contrast, will confirm the diagnosis. The diagnosis is often missed, and late presentations carry a high mortality. Prior to the advent of surgery the condition was universally lethal. Treatment is surgical intervention for most. Occasionally late presentations might be managed conservatively.
* Completely useless afternote: For the food lovers amongst you: his meal consisted of veal soup, cabbage boiled with mutton, calf sweetbreads, spinach, duck, two larks, apple compote, bread and beer. This was followed by Moselle wine, a dessert of pears, grapes and sweetbreads. No wonder he felt sick afterwards! Fred Declerck Nov 2020
0 Comments
|
This will be an archive of learning blogs and lunchtime learnings bites!
Archives
February 2023
Categories
All
|
 RSS Feed
RSS Feed